
The patient information paper on median arcuate ligament syndrome has had a surprising amount of traction. I had Google’s notebook LM create a podcast.
Link to paper in here.

The patient information paper on median arcuate ligament syndrome has had a surprising amount of traction. I had Google’s notebook LM create a podcast.
Link to paper in here.
This article went up earlier this year and it was an oversight to not post it here on my blog. It is an article explaining MALS for the lay public drawn from my clinical experience going back ten years. Our approach is still a work in progress as each patient is comes with a unique presentation. Here is the link
In George Orwell’s Animal Farm, under the dictatorship of the alpha pig, Napoleon, the pigs who represented the nomenklatura of the farm chant the slogan “four legs good, two legs better,” after initially declaring “four legs good, two legs bad” during their revolution. They clearly understood the luxury afforded by a bipedal lifestyle, because in rising on two legs, you get arms and hands which can do many things like caress a baby or wield a cudgel. What the pigs in the parable weren’t realizing were the consequences of a bipedal lifestyle.
When Lucy, the Australopithecine, bipedal hominid ran about on two legs, she did have the use of two arms and hands. Possibly an adaptation to living in tall grasslands with few trees, the ability to stand tall like meerkats, allowed the biped to see far into the horizon for big cats who probably loved the big brained hominid for the high calorie meal inside the hard skull -many fossils from this time show puncture marks from the incisors of medium to large cats.
The walking and running put heat stress on the brain, and the tool use which happened incredibly early and is observed in the chimpanzee, likely drove the selection for a larger brain (more neurons will allow for one to lose some neurons to heat stress but stay in the game), but it created likely the first problem for our ancestors -discharging a cantaloupe sized head through a pelvis that was small to begin with but now also reshaped for bipedalism. We still suffer from a childbirth process that no other mammal faces -birthing a less than fully cooked baby -a tradeoff for that giant head.
Standing also meant the load bearing was shifted 90 degrees with long term consequences. For our ancestors who only lived about 20-40 years if the chimps are correct, this wasn’t a big deal as arthritis and tendinitis didn’t preclude eating and breeding and didn’t affect them until they were old. But with modern sanitation and social structures, we are reaching 100 years and the majority of the problems of the integument -the bones and ligament, the low back pain, the sore knees, the ratchety hips, can all be explained by our bipedal lifestyle. Your arm is 30-50 pounds of meat and bone and supported only by muscles off your spine, and your blood vessels and nerves traverse a narrow passage through these muscles and your first rib. Your diaphragm with 5-10 pounds of heart, lungs, and blood sits on first branch artery off of your aorta. Your veins, designed to drain blood from your organs, have to do so with over a meter of static water pressure and your sump pumps only work when you are walking. Muscles and their tendons are stretched tight in the odd way that upright walking and running demands, compressing blood vessels and nerves. All of this weight is put on your feet which have to deal with up to a ton of pressure with running…
I’ve talked about this concept many times before but never had a chance to put it together like this talk. I may write an article. Looking back, I did this blog post (Link).
I am grateful to Ms. Mei Nortley and Mr. John Raphael for the invitation to give this talk.
A nationwide analysis of median arcuate ligament release between 2010 and 2020: a NSQIP Study
— Read on link.springer.com/epdf/10.1007/s00464-022-09431-3
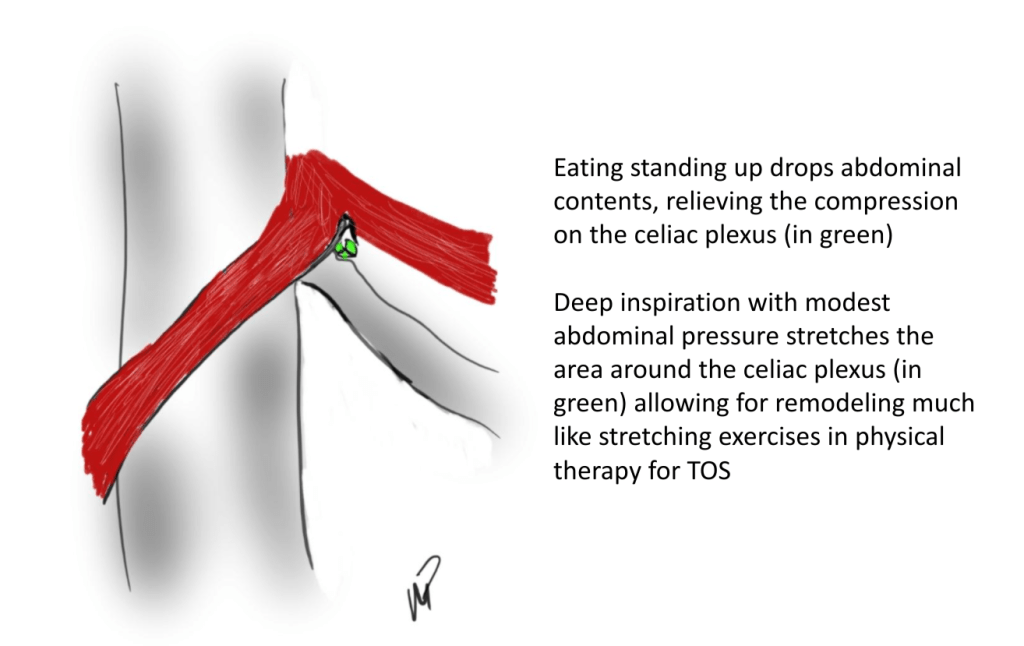
The patient is a young woman who presented with classic symptoms and findings of median arcuate ligament syndrome (MALS). She avoided food because eating triggered severe pain in her upper abdomen. Over a year, this resulted in 15 pounds of weight loss. As a result, she no longer had the energy to work or exercise. She had an extensive gastrointestinal workup including blood work (LFT’s, amylase, cholesterol panel), abdominal CT scan, and upper endoscopy which were normal except for the finding of narrowing of the celiac axis due to compression by the median arcuate ligament. Examination was notable for upper abdominal pain exacerbated by pressure and seated, hunched-over posture. Unfortunately, due to her health insurance, surgery was not covered and she did not want any. So I recommended she try the following.

Over the past several years, I’ve noted that most patients respond to this, even in acute MALS pain situations (yes, there is acute MALS like slipped discs, for another post). That patient came back a few weeks later reporting that she was able to eat more food, more frequently. She also acknowledged compliance with the exercise and postural adjustments at work. A month later she reported regaining her lost weight and only mild pain with sitting in a car for a long time. She was still eating standing up, and she was grateful for having been treated without surgery.
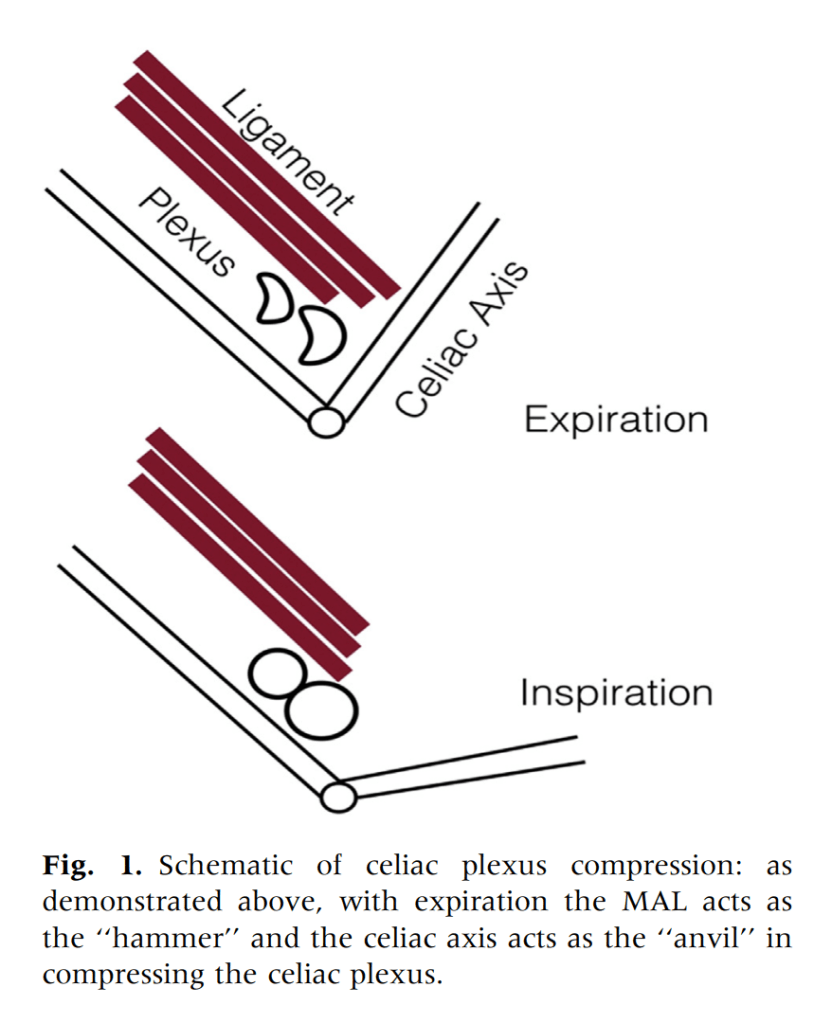
We have postulated that MALS is a nerve compression syndrome of the celiac plexus by the median arcuate ligament (reference). There are two consequences to MALS, neither of which is mesenteric ischemia. The first is this compression of the celiac plexus with injury resulting in inflammation and fibrosis, resulting in further compression and a neuropathy of the celiac plexus. This neuropathy triggers aberrant pain sensations in response to eating. The other consequence is remodeling and injury due to arterial compression. The celiac axis can develop post-stenotic dilatation, growing large enough to be considered aneurysmal. The compression can damage the intima resulting in dissection. The artery can be injured and a pseudoaneurysm can develop. Finally, the aneurysmal segments may develop thrombosis and be the source of thromboembolism, usually to the spleen. Even when the celiac axis clots off, unless there has been resectional surgery such as a Whipple or splenectomy, the stomach gets enough collateral flow that ischemia is rare when celiac axis occlusion occurs. So similarly to thoracic outlet syndrome (TOS), there is a neurogenic MALS and an arterial MALS.
The first line of therapy in neurogenic TOS is physical therapy. With symptomatic MALS, I wondered if there could be physical therapy as well. This young woman and others I have managed nonoperatively suggests good response in some, and partial response in most to exercises and maneuvers designed to address the compression.
Currently, in lieu of celiac plexus block, I have patients treat their MALS nonoperatively using the above protocol for 2-4 weeks, typically while they undergo further workup to rule out more common gastrointestinal etiologies of their abdominal pain, and many have been able to improve their circumstances with these measures alone. This patient chose not to have operation as she was able to live symptom free and regain lost weight with these recommendations alone.

Addendum
I received a comment from Ms. Suzanne Peek, president of the National MALS Foundation, who correctly pointed out not everyone presents in this way. I agree each patient undergoes a unique journey that is often marked by diagnostic delays because this is a rare condition. As I stated, not every patient responds to this regimen and after work up typically will undergo surgery to which in our published results 85% have a positive response to when diagnosed with MALS. Is certainly an area of further study to see if more people can respond to this non-operative approach. Our previous protocol which we instituted after the publication of our report was to use celiac plexus blockade as a diagnostic study and occasionally permanent blockade as therapy for those with prohibitive operative risk. A positive response to this regimen may signal a positive response to surgical celiac plexus ablation.
Reference
Weber JM, Boules M, Fong K, Abraham B, Bena J, El-Hayek K, Kroh M, Park WM. Median Arcuate Ligament Syndrome Is Not a Vascular Disease. Ann Vasc Surg. 2016 Jan;30:22-7. doi: 10.1016/j.avsg.2015.07.013. Epub 2015 Sep 10. PMID: 26365109.

A body floating in space, a fetus in the womb, a dad lounging in his favorite chair, share the feature of weightlessness and represent the absolute neutral position (figure above) of the human which is the position of a relaxed supine quadruped -a dead mouse. Anything else is a stress position, including standing. Repeating motions outside of this relaxed pose or holding those positions away from this absolute neutral for long periods of time is a nidus for injury and pain. That is why most land animals sleep flat on the ground.
The Pain Operations
Operations to relieve pain are often the most gratifying to both patient and surgeon to perform successfully. This circumstance applies to the commonly performed procedures such as spine surgery, endometrial ablations, and varicose vein resections. When the pain is due to a rare set of circumstances, things are not so easy. Typically for rarer pain syndromes, two things need to coincide for the successful operation to happen. First is the patient must suffer while more common and potentially life threatening diseases are ruled out and even treated if these are found. This may take months or years. The second necessary condition is finding a physician who has seen the particular pain syndrome before and understand how to test for it and treat it. That meant the majority of people never get treated, or are shunted into the circle of shame as malingering, drug seeking, and mentally unstable. The opioid epidemic creates double jeopardy for these patients -they can become addicts as their pain is never successfully diagnosed and treated and they get labeled as drug seeking.

All pain syndromes that can be successfully treated share common features that give you a degree of surety about the diagnosis, but at the end, there is a leap of faith on the part of both patient and practitioner because many of these operations have a failure rate ranging from 5-20 percent. First, the symptoms must be associated with sensory nerves, somatic or visceral. Second, there is a physical mechanism for that nerve to be inflamed from compression, swelling, or irritation that can be accounted for through history, physical examination, and imaging studies. Third, though not a constant, a major nerve trunk will be associated with a blood vessel, typically and artery, that is also affected by compression. Fourth, when swollen veins are the cause of pain, it has to be recognized that at an end stage the organ that the veins drain can also be affected.
The Pain Must Have a Testable Anatomic Basis
The somatic sensory nerves in the periphery are well mapped out and known since even classical times. The described pain should be consistent with a nerve. The best and easiest example is a neuroma that forms in an amputation stump. It triggers pain in its former distribution. It is palpable as a nodular mass. It is visible under ultrasound or cross sectional imaging. And it is easy to turn off temporarily with an injection of lidocaine, either under palpation or image guidance. If you can turn off the nerve and relieve the pain, it is likely that ablating or relieving the nerve of irritation will also relieve the pain. Such is the case in median arcuate ligament syndrome (figure below). The celiac plexus is caught under the median arcuate ligament and compressed. It causes a neuropathy that is felt in its visceral sensory distribution and the brain interprets these signals in the typical ways irritation of the stomach is interpreted -as pain, burning, nausea, sensations of bloating, and general malaise. These nerves can be turned off with a celiac plexus block and the effects tested by giving the patient a sandwich. When it works, the patient will say they will have had relief for the first time in years and operation to relieve the ligament compression and ablate the nerve can proceed. Same for many of the diseases listed.
The celiac plexus is caught under the median arcuate ligament and compressed. It causes a neuropathy that is felt in its visceral sensory distribution and the brain interprets these signals in the typical ways irritation of the stomach is interpreted -as pain, burning, nausea, sensations of bloating, and general malaise. These nerves can be turned off with a celiac plexus block and the effects tested by giving the patient a sandwich. When it works, the patient will say they will have had relief for the first time in years and operation to relieve the ligament compression and ablate the nerve can proceed. Same for many of the diseases listed.
Tight Spaces Impinging Nerves, Arteries, and Veins
Many of the tight spaces involving the nerves have accompanying arteries that are compressed. This results in injury to the artery in the form of intimal hyperplasia, post stenotic dilatation, aneurysm formation, and thromboembolism. Shared tight spaces that cause problems for nerves and arteries have the common features of fixed ligaments, adjacent bones and muscles, inflammation, and motion. These include the thoracic outlet, antecubital fossa, cubital canal, diaphragmatic hiatus at median arcuate ligament, inguinal ligament, popliteal fossa, carpal tunnel, obturator canal, mediastinum, retroperitoneum -basically anywhere nerve, compression, and motion occur. In some instances of median arcuate ligament syndrome, postures and breathing trigger the pain. Holding a child in an arm may trigger pain in neurogenic thoracic outlet. Or sitting while wearing tight jeans may trigger a burning pain in meralgia paresthetica. It is not uncommon to find damaged arteries in median arcuate ligament syndrome, thoracic outlet syndrome, and popliteal entrapment or thrombosed veins in nutcracker syndrome, May-Thurner Syndrome, and Paget-von Schroetter Syndrome. Because nerves are typically difficult to visualize, their compression may only be inferred by testing for compression in their adjacent arteries.
Dilated Veins and Swollen Organs and Visceral Pain
Venous hypertension is most commonly conceived of as varicose and spider veins of the legs and offer a model of pain when applied to other pain caused by venous dissension. The visceral sensory fibers veins and arteries trigger a very intense pain that localizes to the trigger. I have often witnessed this when I manipulate a blood vessel during local anesthesia cases. Visceral pain from swelling has a dull achiness that is localizable to my spider veins after a long day standing like a bruise (below). The swelling from varicoceles which I have also had feel nothing less than feeling the aftereffects of getting a kick in the balls -not the immediate sharp pain but imagine about 5 minutes after with the mild nausea, abdominal discomfort and desire not to move too much, and even a little flank pain. Imagine this occurring low in the pelvis with ovarian vein varices in pelvic congestion syndrome. This kind of swollen gonad pain afflicts many women whose pain is so frequently dismissed by male physicians because they have no context -well imagine getting kicked in the balls hard, wait about 5 minutes and that moment stretch it out to whenever you stand for a long period of time (below).
The swelling from varicoceles which I have also had feel nothing less than feeling the aftereffects of getting a kick in the balls -not the immediate sharp pain but imagine about 5 minutes after with the mild nausea, abdominal discomfort and desire not to move too much, and even a little flank pain. Imagine this occurring low in the pelvis with ovarian vein varices in pelvic congestion syndrome. This kind of swollen gonad pain afflicts many women whose pain is so frequently dismissed by male physicians because they have no context -well imagine getting kicked in the balls hard, wait about 5 minutes and that moment stretch it out to whenever you stand for a long period of time (below).
When a limb is swollen from a thrombosis, the veins hurt and is similar to a bone pain from a fracture or a pulled muscle -that is how the brain processes the pain, but when the muscles and skin get tight from edema, the pain is sharp and dire. This is the same kind for pain from a distended left kidney from nutcracker syndrome or a spleen from a splenic vein thrombosis. These conditions can be modeled and predicted based on history and correct differential and confirmed with proper imaging -always.
Build a theory of the pain based on a testable proposition and set of nerves
That is the final message. These pain syndrome require some imagination and empathy to map and model. Predictive tests then can be performed on physical examination, functional testing, or imaging. Often, the adjacent artery is the only thing that can be reliably visualized and tested, knowing that it is the nerve that is compressed. Turning off the offending nerve with a block and relieving the pain is the most powerful argument for operating. It is building the argument for an operation that requires these objective data, but at the end, it does require some experience and faith. You have to believe in your patient and the science and when they coincide, you have to act.
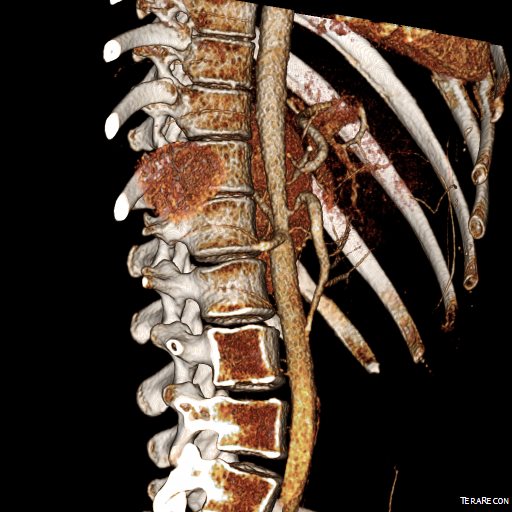
The patient is a young woman from overseas who was referred to the clinic for abdominal and chest pain that persisted after diagnosis and treatment of Takayasu’s Arteritis affecting her visceral (middle) aorta. A year prior to presentation, she had been having severe abdominal pain, 30 pound weight loss, and weakness. Laboratory findings included elevated inflammatory markers. CT scan showed inflammation around her celiac axis and superior mesenteric artery. She was treated with prednisone but only responded ultimately to immunosuppressives. Her pain remitted for a while and she regained weight and strength, but eventually in the months prior to consultation, symptoms of postprandial abdominal pain and nausea set in with concomitant constant midsternal chest pain which at times was incapacitating.
Examination was remarkable for a well nourished young woman in distress with epigastric tenderness. Inflammatory markers were normal and she was on methotrexate and tocilizumab. CTA (above) and duplex showed severe stenoses affecting the origins of the celiac axis and superior mesenteric artery. A composite of the centerlines through these showed the arteries to be critically narrowed at their origins (below), along with a mild to moderate stenosis of the aorta (above). No active inflammation could be seen.
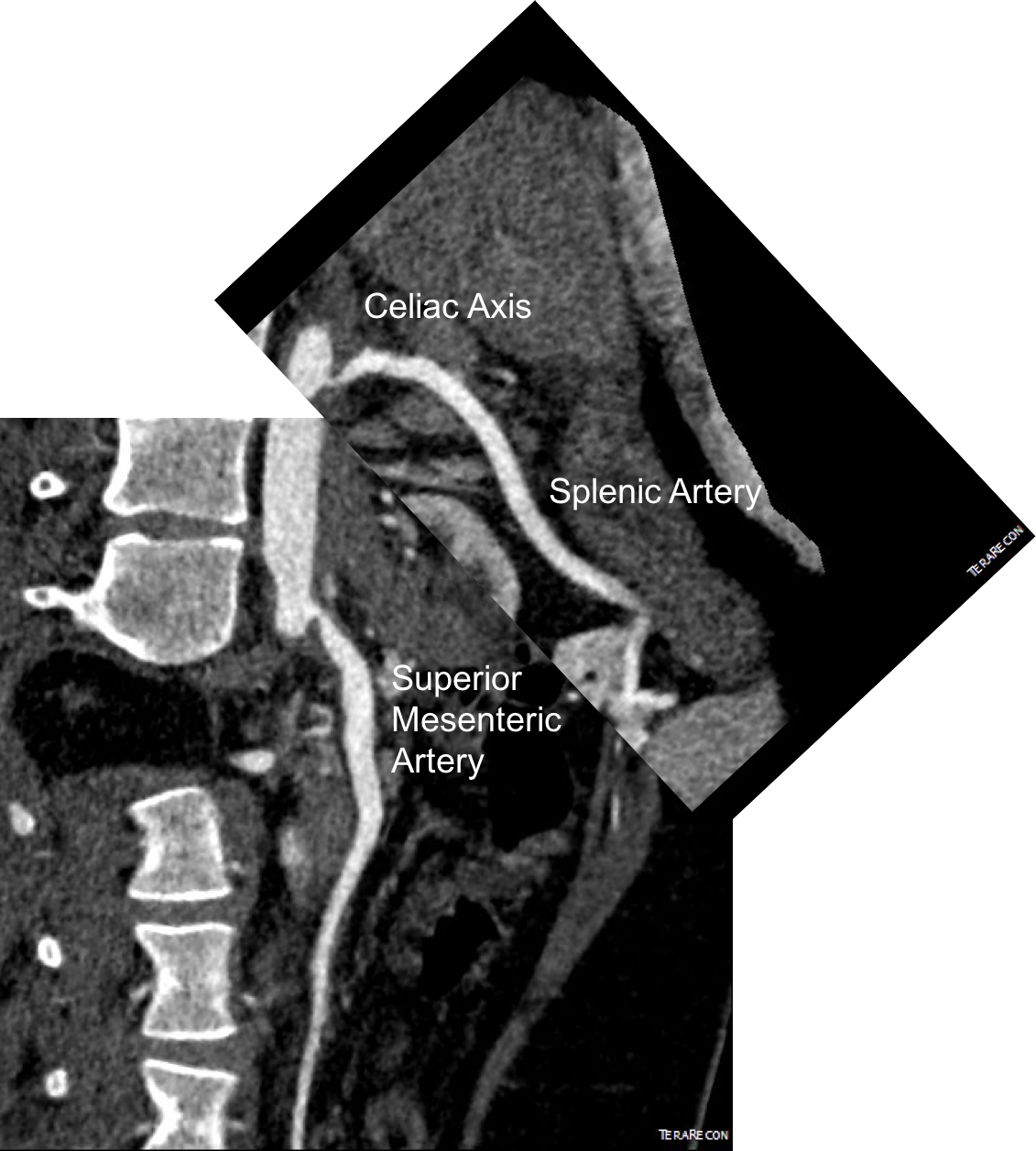
The anterior view of the 3DVR images of her CT showed an absence of collateralization via the inferior mesenteric artery and Arc of Riolan.

This could account for her postprandial abdominal pain which was midabdominal, but the midsternal chest pain was difficult to explain. A cardiac cause had been ruled out at her home institution. It was on the lower part of the sternum and bordered the epigastrium. Through my work with median arcuate ligament syndrome, it was not unusual to have chest pain be part of the pain syndrome which comes about through the compression of the celiac plexus by the median arcuate ligament (reference), and treated effectively with the division of the median arcuate ligament and celiac plexus neurolysis.
I did feel that revascularizing the SMA was likely to improve her postprandial symptoms, given the paucity of circulation to the gut. I had a discussion about her chest pain and the thought that this was a celiac plexus neuropathy as the result of compression of the celiac plexus by her Takayasu’s disease. Typically, for younger people, I perform a bifurcated graft to the celiac axis and SMA from the distal descending thoracic aorta for younger patients, but I had no intention of replacing her aorta at this time, and wanted to reserve any definitive revascularization of her visceral vessels for a later time if it became necessary. Her pulses were full in the legs and she had no hypertension, renal insufficiency, or claudication. I therefore planned a ilio-mesenteric bypass, as it would preserve planes for a later more definitive operation if necessary, and would address her mesenteric ischemia.
I also proposed taking down the median arcuate ligament and lysing her celiac plexus to treat her chest pain symptoms. While I knew this would be fraught with some hazard because of the inflammation that had been there, it would be the best chance at treating this symptom that was debilitating her. I did not think the constant chest/epigastric pain had a vascular etiology. Normally, I would test this with a celiac plexus block, but given the likely inflammation involved, a failed block would not be helpful, and a positive one achieved with some difficulty.
The patient thought this was reasonable and agreed. She underwent a midline laparotomy and I exposed both the SMA and right common iliac artery in the retroperitoneum and tunneled a PTFE graft in a C-pattern in the retroperitoneum. The SMA was diseased proximally under the pancreas and affected by inflammatory scar tissue, and the vessel was thickened as well. The iliac pulse was normal and full and provided excellent inflow.
Going into the lesser sac, the crurae of the diaphragm were heavily scarred near the celiac axis. Division of these fiber was taken slowly and with the aid of both loupe magnification and a hook cautery (borrowed from laparoscopic surgery). The aorta was cleared of tissue first -it was also encased in scar tissue. The dissection going distally was made difficult by inflammatory scar tissue as well, but several large nerve trunks were encountered and divided. The celiac axis was atretic and small within this scar tissue, but was released down to the trifurcation.
The recovery was notable for remission of her chest pain and her ability to resume eating without pain or nausea. A CTA done before discharge showed a patent bypass.

Followup communication has revealed continued remission of her presenting symptoms months after her operation.
We are working on presenting a followup to our recent paper on MALS. Increasingly, it is apparent that consideration of celiac plexus compression as an etiology of epigastric abdominal pain unexplained by more common gastrointestinal causes provides solutions for patients given no explanation for their debilitating pain. This pain can also affect the chest, and flanks and back in the distal thoracic dermatomes, and mimic the some of the symptoms of mesenteric ischemia. In those with recurrent MALS after a successful ligament release and interval of symptom remission, even in the absence of celiac axis compression, a positive response to a celiac plexus block points to the presence of either remnant plexus fibers or compression by scar tissue of the cut nerve endings (neuromata) and reoperation has been successful. Extrapolating this experience to this patient with inflammatory compression of the celiac plexus secondary to Takayasu’s Arteritis made sense and celiac neurolysis appears effective.
Reference
Weber JM, Boules M, Fong K, Abraham B, Bena J, El-Hayek K, Kroh M, Park WM. Median arcuate ligament syndrome is not a vascular disease. Ann Vasc Surg. 2016 Jan;30:22-7.
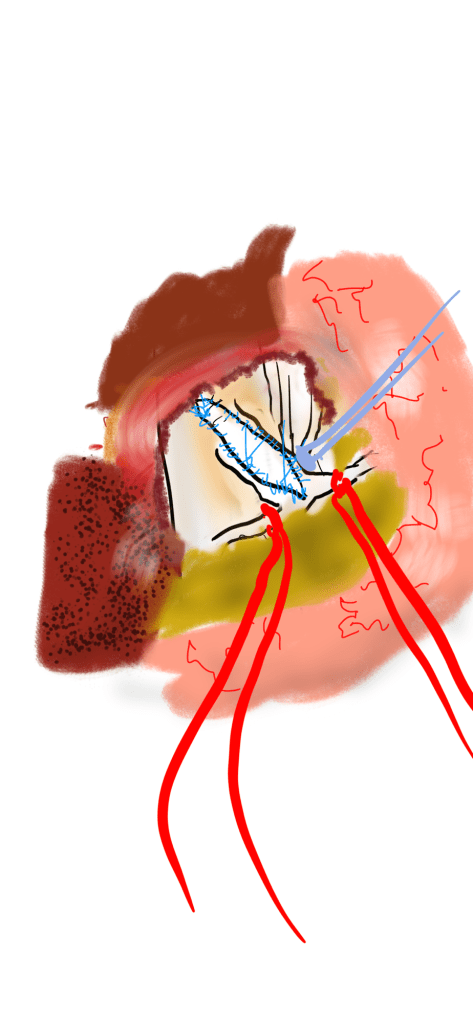
This is a picture from several years ago when I released the median arcuate ligament with open surgery. Seen tented up by the right angle clamp is the fibromuscular tissue over the celiac axis. You can also see a cord of celiac plexus, which gives the foregut somatic sensory innervation. It is becoming clearer that MALS is a nerve compression syndrome in the same way that carpal tunnel compression of the median nerve or thoracic outlet compression of the brachial plexus causes pain. Like nTOS, the arterial compression is a bystander, but a necessary finding in the diagnosis. The celiac axis and median arcuate ligament acts as a nerve compressor. This is why people with MALS respond to celiac plexus block and why it makes sense they don’t have mesenteric ischemia.