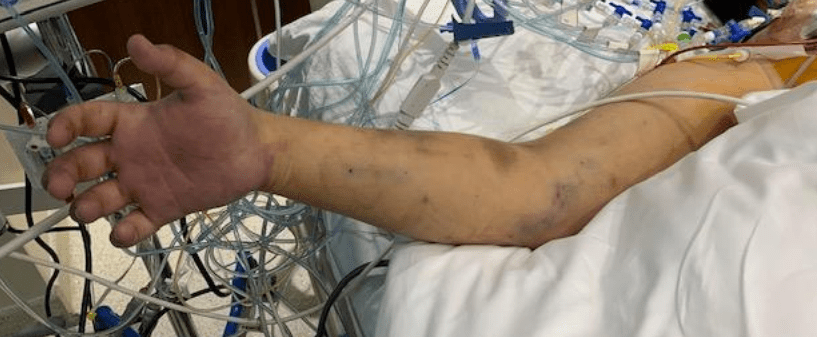
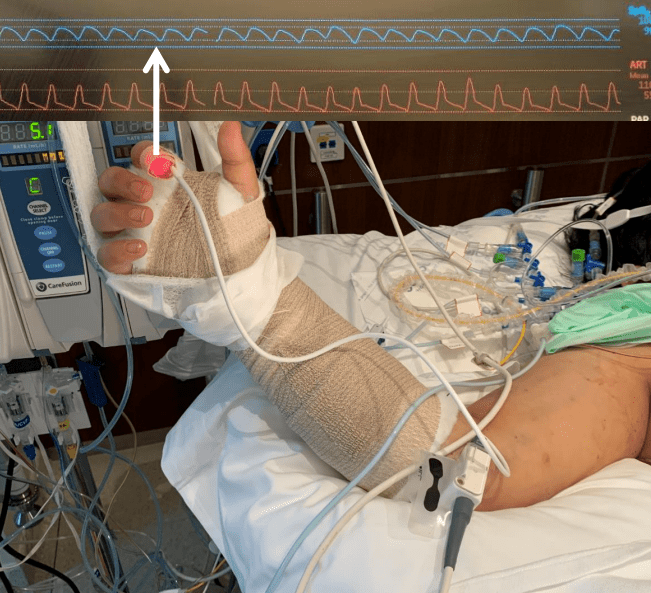
Every time someone on Seinfeld went to the hospital, a stock scene (above) would play. It’s the old ER of Roosevelt Hospital on 9th Ave before the renovations moved it to current 59th street entrance. I was a surgery resident there in the 90’s and watched each Seinfeld episode for the upper West Side stuff that would pop up. The soup Na2i was a few blocks over. Not seen on this pic is the Sym’s operating theater designed by Dr. Charles McBurney which is a designated landmark and currently a private school for “gifted but difficult” children (link). I used to round on patients in the red building -they would be ten in a room separated, if lucky, by rolling privacy screens. My sister was born here. John Lennon died here. All that gone, because hospital buildings are like dressings on a city’s wounds and need to be changed every generation. In fact, it’s not even called Roosevelt Hospital any more.
Roosevelt Hospital’s name was changed to Mount Sinai West, and its sister hospital, St. Luke’s, was changed to Mount Sinai Morningside. I would like to imagine that it was vengeance a century in the making, for pearl clutching slights originating from the gilded age, of blue bloods v. upstart Jews. Because no matter how far you are from the shtetl, there is always another golden door closed to you in New York City. So it seemed for me, an immigrant who had worked hard to get to Harvard College, and Columbia P&S, to look with squinted eyes at my letter on match day and see St. Luke’s/Roosevelt Hospital Center, my last choice that I listed out of a general interest to avoid not matching.
When I landed on St. Luke’s-Roosevelt for my general surgery training, the house officers were quartered in the older parts of the hospital, some rooms dating back to the 19th century, unchanged like unearthed chambers from Pompeii. Both hospitals still had the open wards for the “ward” patients with segregation of the private patients up in the towers. For a time, they still had seamstresses to mend your white coat and cafeterias that still cooked their foods fresh. The resident’s lounge at St. Luke’s was like a frat house common room from the thirties, with a scratched-up pool table, a broken piano, pedastaled hotel ashtrays, and card tables. An old handprinted sign (which I regret not taking) listed the house officer’s rules and entitlements which included two beers or a shot of whiskey per night on call.
After my intern year, both hospitals started sorely needed renovations. The surgery office had to be cleaned out, and behind an antique cabinet, wooden boxes of chromic cat-gut suture were found, still in their glass tubes and preserving fluids, little brown skeins of suture floating like preserved fetuses, a strange message from a faraway time. I ran into Walter Wichern, chairman emeritus, who showed up randomly to the hospital in blue blazer and bow tie. I had just stained my dress shirt pocket with my soon-to-be-lost Mont Blanc fountain pen, and he launched into a story about how he repaired a ruptured aortic aneurysm back in 60’s by cutting his new polyester dress shirt into a tube and sewing a graft out of it down in the laundry, after hearing a talk from Arthur Vorhees at P&S. And he was smiling an enigmatic little smile, recalling how that patient on being discharged gifted him annually with ten new dress shirts every year. I later found out that Dr. Wichern was famously taciturn, and I had somehow unlocked an achievement -getting a story out of an old surgeon. It was around then that I had started to feel that it wasn’t all a big mistake.
When I recently changed hospitals from the Cleveland Clinic to University Hospitals, I had to submit documents for privileging, and I get a testy email. “Where did you do your residency?” The administrator couldn’t find St. Luke’s/Roosevelt anywhere on the ACGME website, or even on Google. When I offered the new names, the reply came back, “They only have records going back to when they took over in 2008.” I briefly contemplated retiring, then asked if sending pictures of my framed degrees would be sufficient. Only partly, was the reply. She wanted witnesses.
My first night on call was terrifying. I was on call with Bobby Borromeo -my fellow intern, Anil Hingorani -our PGY4, and Jesse Jean-Claude -our Chief Resident. All of us are now practicing vascular surgeons -Bobby (fellowship Yale), Anil (fellowship Montefiore), Jesse (fellowship UCSF), and myself (fellowship Mayo), embarked on a night of call that involved no sleep and little food. The single moment I recall was taking Bobby through a blood draw and filling the forms for processing the labs and performing EKGs with an antique strip recorder, cutting and pasting the strips onto a formatted sheet for the chart. Bobby didn’t know how because there were many people to do these things in his home hospital in the Phillipines. For myself, I knew the two hospitals from my rotations during medical school. I could draw blood and cut, sew and tie above my level from my time as a senior student at P&S. I got a bit too comfortable with my privilege, and I was still thinking I should have been somewhere else. Over breakfast, I absentmindedly voiced this out loud and was corrected in a way that is no longer possible in 2022. It was the tone that I remember, of being chewed out.
One of chiefs snapped at me,”You have no idea how big and important these hospitals are. They are older than all the other hospitals here in NY. McBurney did the first appy here. Halsted was chief at Roosevelt and invented cancer surgery and the surgical residency. Green invented the LIMA bypass at St. Luke’s. Our chiefs go to better fellowships year over year than any other hospital in Manhattan. You should be grateful to be allowed to round with us.”

It was by my third year I got used to the 120 hours a week. It is only now a quarter century later, that I value it. I was expending my. youth living and breathing surgery in the latter days of St. Luke’s and Roosevelt Hospitals. I was missing my friend’s weddings, missing time with my wife, seeing New York during the glory of the 90’s through the dank recesses of a trauma bay. I was six figures in debt, but I could take out your appendix in twenty minutes. I had just signed on for a year of research with the peerless Dr. David Tilson and was not looking forward to telling my wife who found the original five year deal of residency interminable. Add to that, two years of fellowship. Walking out on the deck of the call room overlooking the Cathedral of St. John the Divine and Columbia’s campus, listening for the sirens, I really felt the spirit of the hospital.
It’s not the name of the place, neither its splendor nor its comforts, but the commitment of the people in the teams that you build, which allows you to do great things. And yet…