
The patient is a younger man in his twenties who began having dizzy spells associated with near syncope and tunnel vision. He was previously an athlete and was fit and never had such episodes -he had a resting heart rate typically in the 60’s or lower. Workup for arrhythmias was ultimately positive for POTS -postural orthostatic tachycardia syndrome and he was referred to Dr. Fredrick Jaeger of our Syncope Clinic. Tilt table testing the demonstrated the reported tachycardia over 140bpm while upright rising from 60bpm while supine. A radionuclide hemodynamic study (Syncope Radionuclide Hemodynamic Test) showed 54% of his blood volume pooled in his left lower extremity and lower abdomen with upright posture. Air plethysmography (PHLEBOTEST) showed abnormal refill and fill times in both legs and a duplex of the legs showed deep venous reflux in both legs. MRV revealed narrowing of left common iliac vein by the overlying right common iliac artery (May-Thurner’s Syndrome, MTS), and this was where the patient came to my clinic.
The MRV, shown above and below showed the typical pathoanatomy for MTS, but the patient had no symptoms related to left leg swelling, DVT, or varicosities. He did have a reducible left inguinal hernia which was quite tender.

After some deliberation, while not promising anything regarding his POTS, I agreed to proceed with treating his pathoanatomy. Discussion with Dr. Jaeger revealed this: normally about 20% of blood volume parks in the legs with standing which is rapidly dissipated with normal calf muscle pump action. In a subset of patients with POTS, there is a 30-40% maldistribution of blood volume into the legs which may or may not drive the autonomic responses leading to POTS. He has never seen a study result showing a 54% distribution.
It made physiologic and anatomic sense to me to proceed with a venogram and intervention, but I confess I was dubious about any affects I might have on the patient’s POTS and I informed him of it. Also, I recommended seeing a general surgeon for his hernia.
Venography showed obstruction of his left common iliac vein as evidenced by the filling of pelvic and lumbar collateral veins.

Intravascular ultrasound showed the narrowing better and more directly (panel below). The right common iliac artery narrowed the left common iliac vein severely.

A 22mm Wall Stent was positioned across this and dilated with a 22mm balloon in the IVC and an 18mm balloon in the iliac vein. The resulting venogram showed resolution of the obstruction with collateral veins no longer visualized (below).
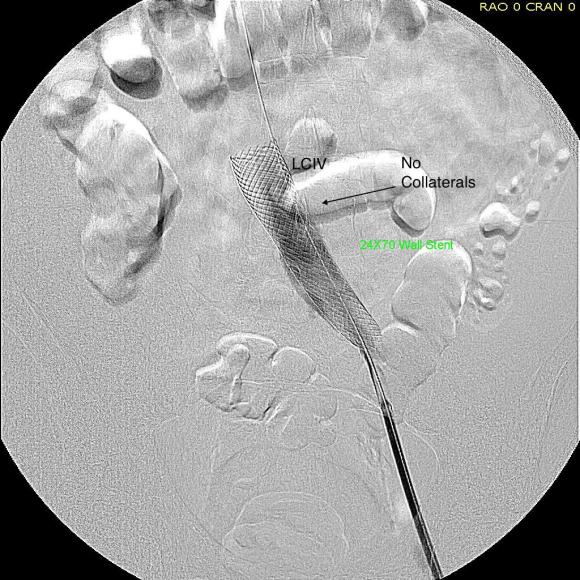
But again, IVUS demonstrated more directly the result (and illustrates the importance of having IVUS available for venous interventions).

The patient was discharged after procedure on a baby aspirin only. He subsequently underwent laparoscopic inguinal herniorrhaphy and returned to my clinic about a month later. His followup duplex showed a widely patent stent and normal flows in the left iliac venous system.
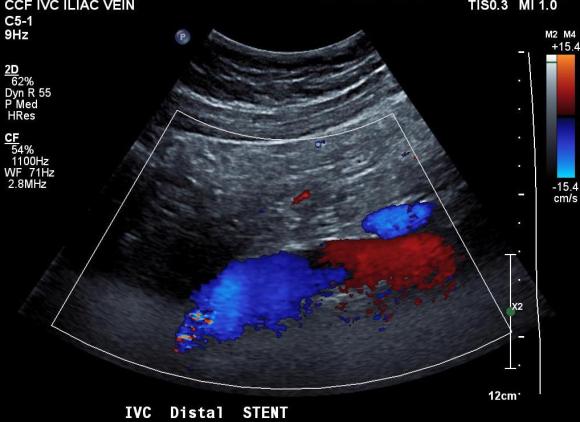
Surprisingly -the patient declared that he was cured of his POTS. He said since the stents went in, he has not had any more episodes of near syncope, dizziness, tunnel vision, nor weakness requiring lying down to rest. His wife confirmed that he was a flurry of activity over the holidays that was surprising considering how debilitated he was before. This is astonishing to me.
But it should not be a surprise given this: if the POTS symptoms were the result of autonomic dysregulation, a breakdown of the feedback control loop, there were only several places this could be a problem.

The pathology, the MTS, explains the POTS in this instance very nicely. Because the problem was in the cardiovascular system part of the diagram which I can fix and not the autonomic nervous system control element, which I can’t fix yet, a solution could be tried. This was not an asymptomatic compression of the iliac vein which we do encounter as an incidental finding. It seems to be POTS caused by MTS, and cured for now by treatment of the MTS.
